Autoimmune disorders: practical signs, treatments, and what to watch for
If your immune system seems to turn on you, you might be dealing with an autoimmune disorder. That’s when the body attacks healthy tissue instead of threats. Conditions range from rheumatoid arthritis and lupus to Hashimoto’s thyroiditis and multiple sclerosis. Symptoms can be subtle at first—tiredness, joint pain, unexplained rashes, or brain fog—and they often come and go.
Common treatments and typical side effects
Treatments aim to reduce immune activity and control symptoms. Doctors often use anti-inflammatory drugs for immediate relief, corticosteroids for flare control, and disease-modifying antirheumatic drugs (DMARDs) or biologics to slow disease and prevent damage. Each approach has upsides and trade-offs.
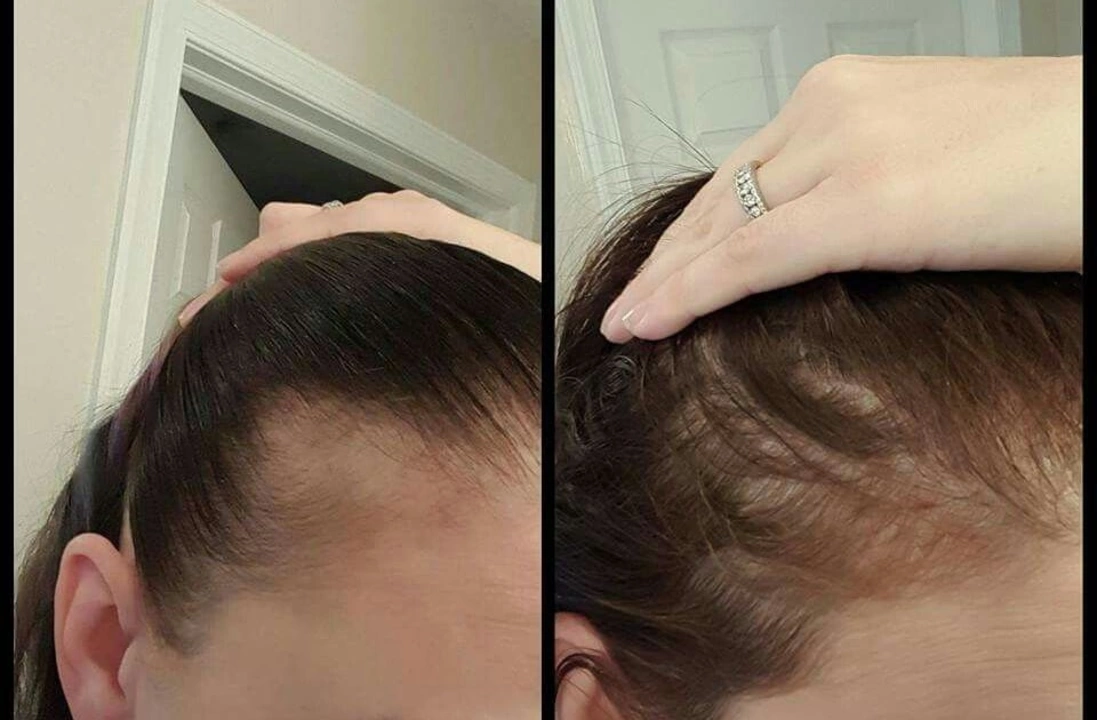
Side effects matter. DMARDs and biologics can increase infection risk and sometimes cause hair thinning or drug-induced alopecia. If you’re worried about hair loss, read targeted guides like “RA Medications and Hair Loss: Methotrexate, Sulfasalazine, Biologics Explained” and “Dermatologist-Approved Treatments for Drug-Induced Alopecia.” Bone health can also take a hit—look into hypophosphatemia and ways to protect your bones if you’re on long-term medication.
Practical tips for daily life and safety
Track symptoms and labs. Keep a short log of flares, new symptoms, and medications—this helps your doctor spot patterns fast. Don’t stop or switch meds without talking to your provider; abrupt changes can trigger flares or withdrawal effects.
Get screened before starting biologics. Some drugs need TB screening or vaccines first. If you live in areas with higher TB risk, you’ll see articles like “Myambutol: Everything You Need To Know About This Tuberculosis Drug” useful for context on TB treatment and testing.
Manage infection risk: wash hands, stay up-to-date on vaccines your doctor approves, and avoid crowded places during heavy immunosuppression. If you notice fever, sore throat, or persistent cough, contact your care team right away.
Be careful when buying meds online. If you need refills or alternatives, use reputable pharmacies and read our safe-buying guides such as “Your Guide to Buying Glyburide Online” or the review of canadapharmacy.com to learn how to spot red flags.
Small lifestyle steps help a lot: steady sleep, gentle exercise (swimming, walking, yoga), and an anti-inflammatory diet can reduce flares for some people. Connect with a specialist—rheumatologists, endocrinologists, or neurologists depending on your condition—and consider a pharmacist or nurse for medication counseling.
Want deeper reads? Check posts under this tag like “RA Medications and Hair Loss,” “Drug-Induced Alopecia,” and “Hypophosphatemia Risks: Protecting Bone Health.” These articles dig into specific side effects, treatment choices, and practical fixes you can try with your healthcare team.
I recently came across a fascinating connection between autoimmune disorders and alopecia, a condition that causes hair loss. It turns out that many autoimmune disorders can lead to alopecia, as they cause the immune system to attack healthy hair follicles. This results in hair loss, either in small patches or across the entire scalp. It's important to consult a medical professional if you're experiencing hair loss, as it could be a sign of an underlying autoimmune disorder. Understanding this link can help raise awareness and lead to better treatment options for those affected.
View Details