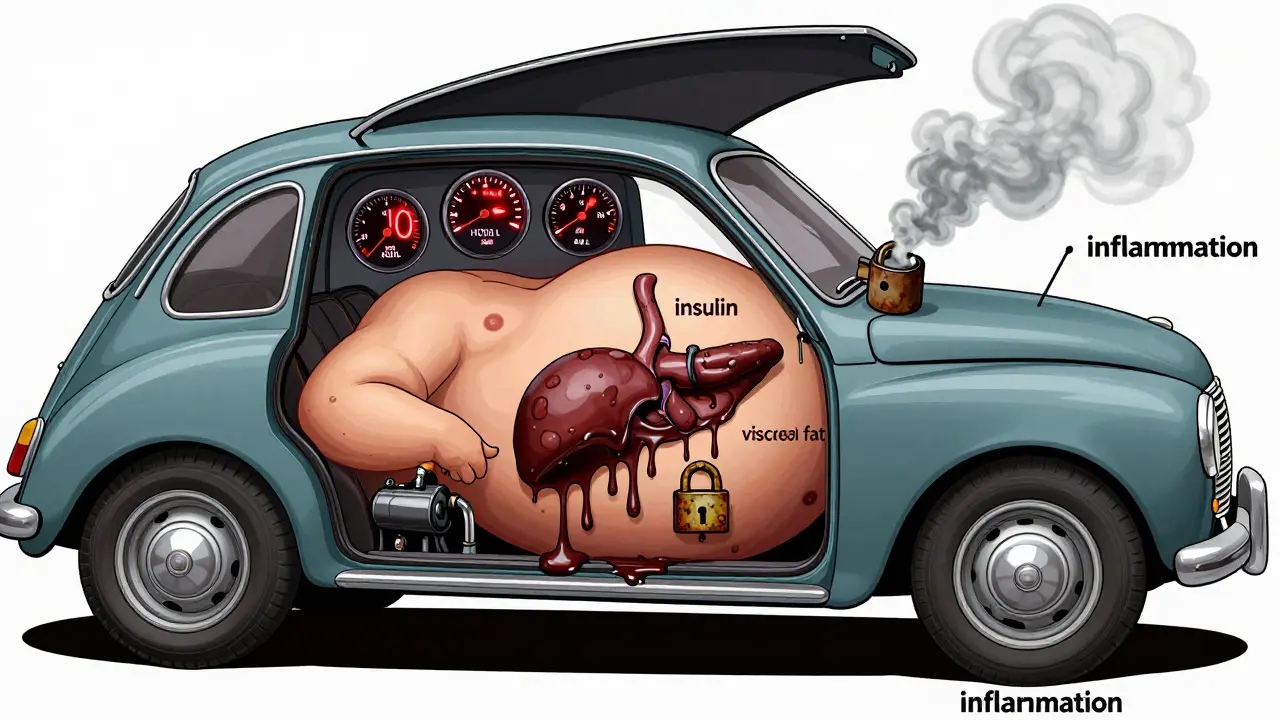
Imagine your body is a car. You fill it with the right fuel, it runs smoothly. But if you keep pouring in cheap gas, letting the oil go stale, and never changing the filters? It starts sputtering. Eventually, it won’t start at all. That’s metabolic syndrome - not one broken part, but the whole system grinding down because of a few quiet, creeping problems: too much belly fat, high blood pressure, and messed-up fats in your blood.
What Exactly Is Metabolic Syndrome?
Metabolic syndrome isn’t a disease you can point to on a scan. It’s a warning sign - a cluster of three or more conditions that, when they show up together, tell you your body’s internal balance is falling apart. The big three? Abdominal obesity, high blood pressure, and abnormal lipids (that’s your cholesterol and triglycerides). Add in high blood sugar, and you’ve got the full picture.
It’s not rare. In the U.S., about 1 in 3 adults have it. In Australia, it’s over 35%. And it’s not just about being overweight. You can be of normal weight and still have metabolic syndrome - if your fat is sitting deep inside your belly, around your organs. That’s the dangerous kind.
The Three Warning Signs You Can’t Ignore
Let’s break down the core components. You don’t need to feel sick to have this. These are numbers your doctor checks - and if three of these five are out of range, you’re diagnosed:
- Abdominal obesity: Waist size over 102 cm (40 inches) for men, or 88 cm (35 inches) for women. For people of Asian descent, the thresholds are lower: 90 cm for men, 80 cm for women. This isn’t about looking big - it’s about fat that’s wrapped around your liver, pancreas, and heart. That fat isn’t harmless padding. It’s active. It releases chemicals that mess with your insulin, your blood pressure, and your fat metabolism.
- High blood pressure: Systolic (top number) 130 or higher, or diastolic (bottom number) 85 or higher. Or you’re already taking medicine for it. This isn’t just about headaches. It’s your arteries under constant stress, wearing down from the inside.
- Bad lipids: Triglycerides at 150 mg/dL or higher. HDL (the "good" cholesterol) below 40 mg/dL for men, or 50 mg/dL for women. High triglycerides mean your body is storing too much fat instead of using it. Low HDL means you’re not cleaning out the gunk from your arteries. Together, they’re a recipe for clogged blood vessels.
- Elevated fasting blood sugar: 100 mg/dL or higher. This means your cells aren’t responding to insulin properly. Your pancreas is working overtime to push sugar into your cells - and it can’t keep up forever.
- Insulin resistance: Not directly measured in routine tests, but it’s the hidden engine behind all this. When your muscles, fat, and liver stop listening to insulin, sugar piles up in your blood. Your body responds by making even more insulin - and that’s when inflammation, fat storage, and high blood pressure start to spiral.
Here’s the thing: none of these alone is a death sentence. But together? They multiply your risk. Someone with metabolic syndrome has double the chance of a heart attack or stroke. Their risk of developing type 2 diabetes jumps by five times.
Why Belly Fat Is the Real Culprit
Not all fat is the same. Fat on your hips? It’s mostly storage. Fat around your waist? That’s visceral fat - the kind that wraps around your organs like a toxic blanket. This isn’t just a cosmetic issue. Visceral fat cells are screaming. They pump out inflammatory chemicals - cytokines, leptin, resistin - that confuse your body’s signals.
Think of insulin like a key. It unlocks your cells so sugar can get in for energy. But with too much visceral fat, the locks get rusty. Your cells don’t open up. Sugar stays in your blood. Your pancreas cranks out more insulin to force the door open. That’s hyperinsulinemia. And that extra insulin? It tells your liver to make more triglycerides. It tells your kidneys to hold onto salt - raising your blood pressure. It tells your body to store even more fat. It’s a loop. And it’s silent.
That’s why waist size matters more than weight. Two people can weigh the same. One has a 90 cm waist. The other has 75 cm. The first one? High risk. The second? Not so much. Your waistline is the most visible clue to what’s happening inside.
Who’s at Risk?
It’s not just about age or laziness. While metabolic syndrome gets more common as you get older - over half of people 60+ have it - it’s hitting younger people harder than ever. Sedentary jobs, constant stress, sugary drinks, and ultra-processed foods are the new normal. But genetics play a role too. People of South Asian, Hispanic, African American, and Indigenous descent face higher risks, even at lower body weights.
Women with PCOS (polycystic ovary syndrome) are at especially high risk. Hormonal shifts change how fat is stored and how insulin works. So are people who’ve had gestational diabetes - even if they lost the baby weight.
And here’s what nobody talks about: you don’t feel this coming. No pain. No warning buzz. Just a slowly rising waistline, a routine blood test that says "elevated triglycerides," or a blood pressure reading that creeps up year after year. That’s why it’s called a silent killer.
How Do You Fix It?
There’s no pill for metabolic syndrome. No magic supplement. No quick fix. The only proven treatment? Lifestyle changes - and they work better than most drugs.
Weight loss of just 5-10% of your body weight can reverse most of the markers. Lose 10 pounds if you’re 200? That’s enough to drop your triglycerides, lower your blood pressure, and improve your insulin sensitivity. You don’t need to be thin. You just need to move the needle.
Move more. Aim for 150 minutes a week of moderate activity - brisk walking, cycling, swimming. You don’t need a gym. Just get your heart rate up. Studies show even breaking it into 10-minute walks helps. Movement pulls sugar out of your blood without needing insulin. It’s like a natural drug.
Eat differently. Cut out sugary drinks. Ditch processed snacks. Reduce refined carbs - white bread, pasta, rice. Replace them with vegetables, legumes, whole grains, lean proteins, and healthy fats (nuts, olive oil, avocado). A diet rich in fiber slows sugar absorption and reduces inflammation. The Mediterranean diet isn’t trendy - it’s backed by decades of data showing it reverses metabolic syndrome.
Stop smoking. Smoking damages blood vessels and makes insulin resistance worse. Quitting is one of the fastest ways to improve your lipid profile and blood pressure.
Medication? Only if needed. If your blood pressure stays high, your doctor might prescribe an ACE inhibitor. If triglycerides are sky-high, statins or fibrates might help. If blood sugar is creeping up, metformin can improve insulin sensitivity. But none of these replace the foundation: food, movement, and weight loss.

What Happens If You Do Nothing?
Left unchecked, metabolic syndrome doesn’t just stay the same. It progresses.
Your insulin resistance gets worse. Your pancreas burns out. Type 2 diabetes follows - often within 5 to 10 years. Your arteries stiffen. Plaque builds up. Heart attack or stroke becomes far more likely. Even if you avoid those, you’re at higher risk for fatty liver disease, kidney damage, and sleep apnea.
And here’s the brutal truth: the longer you wait, the harder it gets to reverse. Each year of high blood sugar, high triglycerides, and high blood pressure leaves a mark. It’s not reversible damage - it’s accumulated wear. The sooner you act, the more you save.
What Should You Do Now?
Step 1: Check your waist. Use a tape measure. Don’t guess. Wrap it around your belly, just above your hip bones. If it’s over 102 cm (men) or 88 cm (women), you’re in the danger zone.
Step 2: Look at your last blood test. Did you have high triglycerides? Low HDL? High fasting glucose? Even one of those is a red flag. Two? You should be concerned. Three? You likely have metabolic syndrome.
Step 3: Talk to your doctor. Don’t wait for symptoms. Ask for a full metabolic panel. Get your blood pressure checked properly - not just once, but over time. Ask about insulin resistance markers if you’re at risk.
Step 4: Start small. Swap one sugary drink for water. Take a 20-minute walk after dinner. Cut out one processed snack a day. You don’t need a complete overhaul. Just one change. Then another. Progress, not perfection.
Metabolic syndrome isn’t your fault. But it’s your responsibility. It’s not about willpower. It’s about understanding how your body works - and giving it what it needs to heal.
Can you have metabolic syndrome without being overweight?
Yes. While most people with metabolic syndrome carry excess weight, it’s possible to have it at a normal BMI if you have high visceral fat - often called "skinny fat." This is common in people with sedentary lifestyles, high sugar intake, or genetic predispositions. Waist circumference is a better indicator than weight alone.
Does metabolic syndrome always lead to diabetes?
No, but it greatly increases the risk. About 5 out of every 100 people with metabolic syndrome develop type 2 diabetes each year. Without intervention, up to 70% will develop it within 10 years. Lifestyle changes can cut that risk in half or more.
Can medications cure metabolic syndrome?
No. Medications can treat individual components - like high blood pressure or high cholesterol - but they don’t fix the root cause: insulin resistance and visceral fat. Lifestyle changes are the only proven way to reverse the syndrome itself. Drugs help manage symptoms, not cure the condition.
How long does it take to reverse metabolic syndrome?
With consistent lifestyle changes, improvements can be seen in as little as 3 months. Blood pressure, triglycerides, and insulin sensitivity often improve quickly. Reversing the diagnosis - meaning you no longer meet three or more criteria - typically takes 6 to 12 months of steady effort. Weight loss of 5-10% is usually enough.
Is metabolic syndrome the same as prediabetes?
Not exactly. Prediabetes means your blood sugar is elevated but not yet diabetic. Metabolic syndrome includes prediabetes as one possible component, but also requires at least two other factors - like high blood pressure or bad cholesterol. You can have prediabetes without metabolic syndrome, and vice versa. But if you have both, your risk is much higher.